How process intelligence holds the key to excellence
As Deming said, “If you can’t describe what you are doing as a process, you don’t know what you’re doing.”
✓ Healthcare Patient flow – track the journey of patients through the healthcare system and identify blockers and opportunities for greater efficiency and better patient care
✓ Call handling – understand talk time, post processing (wrap), rest breaks and much more across call type, department and down to individual agents
✓ Procurement – Understand and optimise your procurement processes across your organisation
✓ Logistics/supply chains – get the right quantity and quality of materials (or services) to the right place at the right time, for the right client, and at the right price
✓ HR (payroll, recruitment) – visualise processes and seek to optimise and provide improved SLA compliance. Optimise and track employee lifecycles;attracting, selecting, training
✓ Customer journeys – create a customer journey map, a visual story of your customers’ interactions with your brand or service and optimise the satisfaction and outcomes delivered
✓ Customer complaints – map the complaints journey and service recovery opportunities across your organisation
✓ Health and safety – visualise and map your health and safety processes, ensuring compliance, efficiency and learning
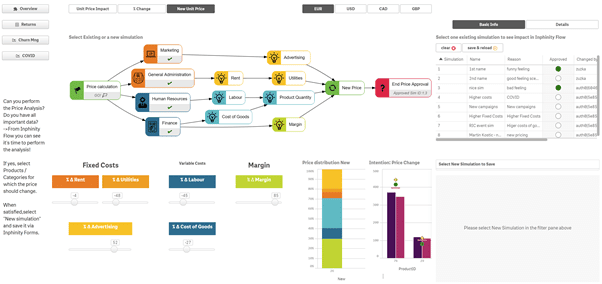
You can only start to ask questions of your process when you can see it. The first stage is to visualise your processes. Your journey of discovery starts here. Once you have mapped your process, you can start to understand the efficiency through measurement.
Design your process KPIs to understand volumetrics, flow, and efficiency. Variation and opportunity for improvement across people, process and system will become visible. Imagine having the process intelligence to identify which parts of the process are clunky and time consuming, and what resources are outliers compared to peers. The aim is to simplify the process steps and reduce the variation in people productivity. Getting control of your processes is the fundamental step towards improved assurance. You can even set alerts for when the process moves outside standardised control values.
As Jack Welch said, “An organization’s ability to learn, and translate that learning into action rapidly, is the ultimate competitive advantage.”
Process improvement is a science, but also an art. Having spent many years running teams to collaboratively map, identify and optimise processes, the ability to add and socialise professional context is paramount. Colleagues across an organisation can add professional context such as data, text and documents to any area. Discussion, ideas and opportunities can be collaborated through workflows and approvals in a simple and powerful way – removing traditional spreadsheet and email procedures.
Monitoring and acting on the process ‘as is’ provides some great opportunities for improvement. But what about looking ahead more and modelling process change. A unique opportunity exists to look at the current state and then model the process efficiency, costs and effectiveness of a future state. What if 10% of your people reduced their time spent processing claims? Improving quantity, quality and reducing costs is fundamental to improved performance.
Having visibility and control over your processes provides a fundamental shift in organisational assurance. Excellence does not happen by chance. Process intelligence provides an opportunity to push the boundaries of excellence!
Working in healthcare currently, must feel like an insurmountable challenge. Unprecedented times. Trying to balance Covid 19 and BAU is stretching the service to the full – and creating ethical dilemmas by the bucket load: Who is a priority? Who has the highest risk? Who is escalating in risk? What have we missed? Hearing the plight of clinicians and patients (and families) is heart breaking. Of course, for every story of pain and suffering, there are 10 good ones. You rarely hear about these in the same way.
Having worked in healthcare with colleagues across the world, seeing success and where the improvements need to be made, it was interesting to be part of the healthcare system over the Christmas period. Firstly, I am forever grateful for the professionals who deal with the most traumatic of circumstances, whilst managing their own wellbeing. The worry of missing something or prioritising one patient over another is hard mentally.
So, as waiting lists are stretched due to the impact of Covid, the question is how do you manage and sustain BAU? Waiting for the resources to gallop over the hill is an unlikely prospect. So where does that leave us?
The first thing to do is truly understanding everything about your organisation: Process, people, and system. Its complex with hundreds of functions trying to operate in an efficient and integrated way. Without analytics shining a light through the organisation, optimising a healthcare system is very hard indeed. Data provides a golden connecting thread. Modern analytics can provide a huge opportunity to get a baseline understanding to support efficiency and effectiveness not seen before. Multiple systems and data sources need to be combined to provide a holistic, contextual 360 view of delivery. Key areas to understand include:
✓ Mapping processes e.g. patient flow
✓ Understanding process bottlenecks and opportunities
✓ Understanding and forecasting demand, capacity and capability
✓ Understanding productivity and how to increase it
✓ Measuring risk and escalation to aid prioritisation and compliance e.g. outpatients waiting lists, readmission, LOS etc
✓ Alerting to provide safety nets and early intervention opportunities
✓ Understanding and improving efficiency e.g. theatre utilisation, bed management
✓ Ensuring accurate financial planning, coding and cost recuperation
✓ Learning from successful outcomes e.g. clinical variation
✓ Understanding and improving data quality
✓ Bringing professional judgement into the analytics to support better context, decisions and action
✓ Understanding population health risks and early intervention opportunities across Integrated Care Systems
At a strategic level, how do your chief operating officers, directorate heads, managers and supervisors assure delivery and mitigate inherent risks associated against a high demand operational arena? It can be often a difficult and time-consuming process. Significant hearsay forms part of the decision making – things get missed.
Achieving assurance across the healthcare can be significantly bolstered by getting the following technology in place:
- Data integration
- Data cataloguing
- Self-serve analytics
- Advanced analytics e.g. predictive, prescriptive
All of these areas can be built into to a Command Centre approach – physical and virtual. For example, Morecambe Bay University Hospital Trust has developed a command centre structure, providing the lynchpin for how resources are optimised. From the emergency department to inpatients ready for discharge, the hub has been designed to give a tangible flow of insight to increase patient safety and experience. As a result, any employee from leadership to clinicians at the coal face can consume the data easily. With this new structure, the Morecambe Bay team holds short, focused, evidence-based staff meetings regularly throughout the day to get updates using live data.
Such transparency of information and the availability of analytics contributes to enhancing healthcare employees’ ability to work with data – improving their data literacy and giving them the means to thrive. Data-savvy organisations in the industry that are looking to adapt their workflows based on available data should first ensure that they get feedback from operational and clinical staff just as much as the IT team, to make sure that any results from changes to such a dynamic working environment can be maximised.
The next level is applying some 4th gen analytics where people are brought into the analytics value chain. When technology and people come together, the magic starts to happen. Enabling healthcare practitioners to see, interact and then ADD context to support better outcomes, across an entire organisation, becomes a real game changer.
There are several factors that have contributed to the evolution of working practices in the healthcare industry, but the omnipresence of data has proved to be the most important catalyst, evolving from the muse of the IT team to something which has become mission critical – a concrete and tangible impact on how staff go about their daily working lives. By merging human and technical factors with immersive tools that allow healthcare workers to integrate data into their decision making, the industry can relieve some of the pressure on it by ensuring staff at all levels are equipped to respond to whatever is thrown at them. Recent examples of using write-back tools to support rapidly changing Covid requirements is a good example.
As the world moves forward, treatment will grind services down to a point of surrender. Prevention is key. To create a sustained and successful health system, we must reduce demand, risk and harm – at the earliest point possible. This is the holy grail for an Integrated Care System. Getting a successful joined up approach between agencies, again will rely on analytics providing the golden thread to support understanding, risk identification, priority, better decision making and ACTION.
All the analytics technology is there right now. Experts are ready to support transformation, the front line is thirsty to consume it. This just needs to be led by innovative and collaborative data driven leaders. Are you one of these people?
WRITTEN BY
Sean Price
VP of Industry Solutions